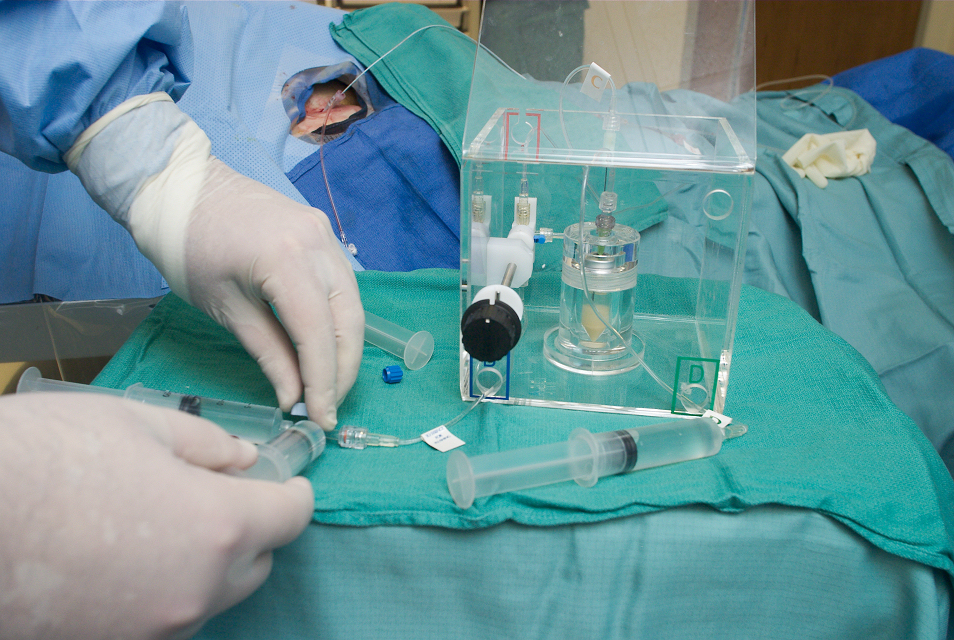
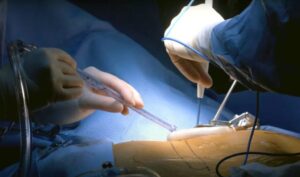
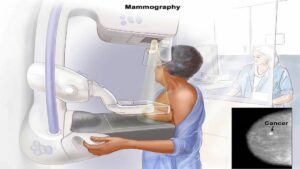
SIRT is a form of cancer treatment, using small radioactive particles that is injected directly into the hepatic artery to target liver cancers. Routinely performed since 2008 in Singapore, it is a minimally invasive specialized cancer treatment that has shown good efficacy and safety, with less side effects as compared with traditional chemotherapy.
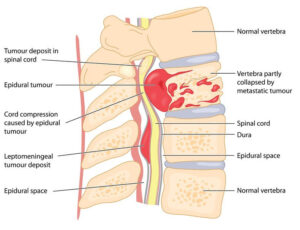
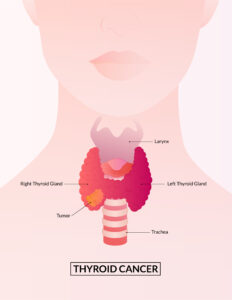
The treatment is indicated for patients with primary liver cancers (for example hepatocellular carcinoma and cholangiocarcinoma) or metastatic disease to the liver (for example colon carcinoma), for whom curative surgery is not an option.
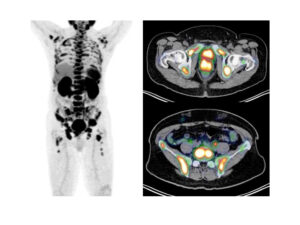
SIRT is used to control the disease, with possibility of downstaging the cancer for surgery in a number of cases. To increase the safety and efficacy of the treatment, an assessment is performed for the patient to determine suitability for SIRT, and to calculate the radiation dose needed. Each treatment is personalized for every patient, and Singapore is the pioneer for artery specific partition modelling dosimetry, which is an advanced technique to calculate tumor specific dosing.
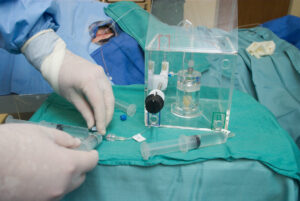
SIRT is a complex procedure requiring multiple different specialists. The team at Farrer Park Hospital is experienced, and has performed more than 40 cases since 2017, with no major complications from SIRT treatment encountered to date.